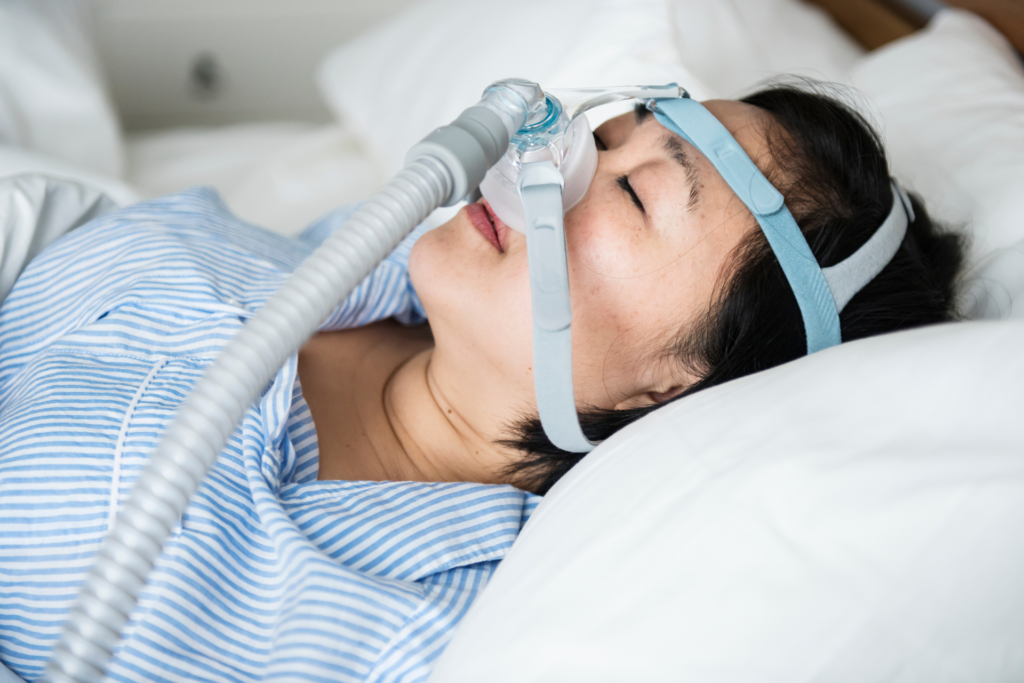
While sleep apnea is often considered a “male” disease, sleep apnea symptoms in women are often left untreated due to a difference in symptoms and causes.
The common trope of associated with sleep apnea is a husband’s loud snoring, with an exasperated wife heading to the couch to get some much-needed sleep. Come morning, both are feeling exhausted and sleep-deprived. After some bickering, they finally decide to do something about the husband’s snoring.
Sleep apnea is often considered a “male” disease, but sleep apnea can and does affect both women and men. From hormones to physiology, sleep apnea symptoms in women are often different than those in men because of biological differences between the genders.
We talk about sleep apnea a lot on our blog, so if you want to learn more, we recommend checking out some of those other articles once you’re done here.
Let’s get right into what causes sleep apnea symptoms in women and men both.
What Causes Sleep Apnea Symptoms in Women and Men?
The most common cause of sleep apnea in all patients is the relaxation of throat muscles.
When the muscles in the back of your throat relax, they narrow or obstruct your airways. This prevents you from getting enough air while you sleep, reducing the oxygen level in your blood. When this happens, your brain wakes you up to help you breathe normally again. These interruptions tend to be so brief you don’t even realize they’re happening.
A sleep apnea sufferer can experience as few as five or even more than 30 of these breathing interruptions per hour!
The causes of these breathing interruptions can vary between women and men. A study from the Sleep Medicine Review outlined their findings about the gender differences in obstructive sleep apnea. [1]
Let’s go through the major causes one by one.
Sleep Apnea & Physiology
Excess weight and obesity are one of the main risk factors for obstructive sleep apnea. The excess weight on your body, around your neck, and the fat around your tongue can obstruct your airways while you sleep. These cause the characteristic breathing difficulties and interruptions of sleep apnea. This is true of both genders.
However, the study identifies that women are more likely to have a body mass index (BMI) greater than or equal to 30, indicating obesity. However, fewer women than men had sleep apnea among these participants.
Researchers believe that fat distribution may be more of a risk factor for sleep apnea in women than weight alone. For men, fat around the tongue can cause airway obstruction. However, this is less common in women with sleep apnea. On top of that, women have a shorter oropharynx than men do. This means that women have a smaller space in their throats at risk of being obstructed or collapsing.
Inversely, fat distribution in men tends to lean more towards the upper body than the lower body, making them more likely to have more fat in their necks than women.
Hormones’ Effect On Sleep Apnea
Hormones like melatonin are vital to a good night’s sleep, and a good night’s sleep is vital to balancing your body’s hormones. This cyclical nature can mean having problems with one can cause problems with the other.
Changing hormone levels is another common cause of sleep apnea, especially for women.
For many women, the onset of menopause also means that they’re more likely to experience sleep-disordered breathing. Postmenopausal women are also more likely to have sleep apnea than premenopausal women. In fact, in comparing the two, OSA was much rarer in premenopausal women (20%) than it was in postmenopausal women (between 47 and 67%). Premenopausal women with obstructive sleep apnea are more likely to have the condition because of obesity or because of the structure of their facial bones.
Different hormones, such as leptin and insulin, also impact how fat is distributed throughout the body.
Postmenopausal women also have higher fat mass than premenopausal women. This fat also tends to exist more in a postmenopausal woman’s upper body than her lower body, increasing her risk of sleep apnea.
Another significant hormone shift can cause obstructive sleep apnea, but this exclusively impacts women.
Related: The Connection Between Sleep Apnea and Hormones
Sleep Apnea & Pregnancy
An expectant mother’s hormone levels change dramatically during pregnancy. A woman’s diaphragm may also elevate as a consequence of her uterus growing during gestation. Fluid retention during pregnancy can also contribute to sleep-disordered breathing and sleep apnea.
Pregnant women also tend to have a larger neck circumference than women who are not pregnant. This can be caused by fluid retention or normal pregnancy weight gain. Women typically gain between 25 and 35 pounds during pregnancy, which can also contribute to narrowing airways and sleep-disordered breathing.
If you’ve ever been pregnant, you may have also noticed a persistent stuffy nose that just wouldn’t go away. It’s also common for pregnant women to experience pregnancy rhinitis, or nasal congestion that only occurs during pregnancy. This congestion can occur both during the day and at night, making it harder for expectant mothers to breathe through their nose while they sleep. [2]
For many women who experience OSA during pregnancy, their symptoms thankfully go away after delivery.
Aging
For both men and women, normal aging comes with physiological changes that can put you at risk for sleep apnea. If you are 55 or older, you are more likely to have an increasing amount of fat around your neck as you age, regardless of your body mass index (BMI), contributing to OSA symptoms.
In one study observing 427 participants between 65 and 95 years old, researchers found that 70 percent of the men and 56 percent of women had obstructive sleep apnea. [1]
Sleep apnea risk only grows as people age, but the specific causes OSA in older adults can also vary by gender. For example, how certain tongue muscles respond to negative pressure— breathing— can make a man’s airway more prone to obstructing or collapsing. In women however, researchers found that women’s soft palate size often increased with age more often than men’s did. This, of course, can also cause airway obstruction.
The Dangers of Untreated Sleep Apnea
For both men and women, sleep apnea is a common cause of excessive daytime sleepiness, morning headaches, and of course, poor sleep. Untreated sleep apnea can also cause or worsen serious, long-term health issues, including:
- Poor heart health, including heart disease, and higher risk of a heart attack or heart failure
- Diabetes
- Obesity
- High blood pressure
- Mental health disorders like depression and anxiety
Even more concerning, between 80 and 90 percent of people with sleep apnea aren’t aware that they even have it. Sleep apnea symptoms occur at night while you sleep, so you may not even be aware that anything is amiss. Remember earlier when we were talking about OSA sleep interruptions— they’re often so brief that you don’t even realize that they’ve happened.
Unless your sleep partner can feel the house shaking when you snore, you probably won’t even be able to detect the most well-known symptom of all: the loud snoring.
So if men and women are both vulnerable to sleep apnea, why is it often seen as a “men-only” disorder? Unfortunately, it’s because men are more likely to get tested and diagnosed than women. This is even considering the relatively few people who are actually diagnosed.
Remember, though, undiagnosed sleep apnea can cause a lot of potential health problems. And for women, this may even include cancer.
Obstructive Sleep Apnea, Cancer Risk, and Gender
According to the American Academy of Sleep Medicine, the link between sleep apnea and cancer may even be stronger in women. This is especially notable because obstructive sleep apnea is more commonly diagnosed in men.
Obstructive sleep apnea occurs in about 24 percent of men and about 9 percent of women. Even if women remain cautious of common risk factors such as weight and tobacco use, they are still two to three times more likely to get cancer than men.
However, more research is needed to determine why women with sleep apnea are at a higher risk for cancer. In fact, there is no known direct causal relationship that links sleep apnea and cancer in women.
A study from the European Respiratory Journal also noted that while more “classic” sleep apnea symptoms like daytime sleepiness and snoring were reported more often in men, women were more likely to experience less obvious symptoms like fatigue, morning headaches, insomnia, and depression. [3]
This is why it’s so important to get tested and treated for obstructive sleep apnea if you believe you may be at risk! This is especially crucial if you are an older man or a postmenopausal woman struggling to get a good night’s sleep.
Related: What You Need to Know About Sleep Apnea and Cancer Risk
CPAP: The Best Treatment for Obstructive Sleep Apnea
Even with a formal diagnosis, sleep apnea won’t go away independently. Once you’ve been diagnosed with sleep apnea, your doctor or a sleep specialist will likely prescribe CPAP therapy to treat the disorder.
CPAP, or continuous positive airway pressure, is the most common and most popular sleep apnea treatment. That’s because it’s also the most effective and least expensive sleep apnea treatment and the only treatment with a long history of documented evidence of helping other conditions such as high blood pressure, diabetes, and cardiovascular disease.
The short explanation why is CPAP therapy ensures that your airway stays open while you sleep and helps you breathe normally all night, even if you have severe sleep apnea.
CPAP machines use a continuous stream of air to gently hold your airways open and prevent them from becoming obstructed. This allows you to breathe normally and sleep peacefully throughout the night.
If you’re unsure where or how to seek treatment for obstructive sleep apnea, you may be wondering— where do you start?
Men are from Mars, Women are from Venus (But Both Are at Risk of Sleep Apnea)
Sleep apnea is considered by many to be a “male” disease, but not only is this sentiment inaccurate, it ignores a myriad of sleep apnea risks faced by women. What causes sleep apnea symptoms in women can be significantly different than what causes these symptoms in men, but being aware of these symptoms can make it much easier for women at risk of sleep apnea to get the treatment they need.
Take our sleep apnea quiz if you think you’re at risk for sleep apnea. It can help you make better sense of your symptoms so you can discuss them with your doctor or a sleep specialist. They may recommend an overnight sleep study to evaluate your sleep patterns or a home sleep apnea test to identify what’s causing your sleep problems.
If you’re worried about your sleep health, contact the Sleep Centers of Middle Tennessee today to schedule a consultation. You shouldn’t have to jump through hoops to get a good night’s sleep— we can help you get back to the restful sleep you deserve.
Citations
1. Lin, Christine M, et al. “Gender Differences in Obstructive Sleep Apnea and Treatment Implications.” U.S. National Library of Medicine, Sleep Medicine Reviews, Dec. 2008, www.ncbi.nlm.nih.gov/pmc/articles/PMC2642982/.
2. “Pregnancy Rhinitis: How Congestion during Pregnancy Is More than a Stuffy Nose.” SinuSonic, SinuSonic, 15 Aug. 2022, sinusonic.com/blogs/learn/pregnancy-rhinitis.
3. Pataka, Athanasia, et al. “Cancer Prevalence Is Increased in Females with Sleep Apnoea: Data from the ESADA Study.” European Respiratory Society, European Respiratory Society, 1 June 2019, erj.ersjournals.com/content/53/6/1900091.